The treatment horizon for bleeding and clotting disorders looks remarkably different than it did just a few years ago. Imagine a future where managing a chronic blood condition is as routine as an annual check-up, rather than a cycle of frequent infusions and emergency room visits. This "future-forward" shift is already underway, transforming how we perceive the internal rivers of our vascular system. With more than 1,000 distinct types of blood disorders identified globally, the complexity of hematology can feel overwhelming. Yet, whether we are discussing the 3.2 million Americans living with anemia or those managing rare inherited conditions, the goal remains the same: stabilizing the delicate balance of our "living pharmacy" to ensure long-term vitality.
Inherited vs. Acquired: Why Do Blood Diseases Occur?
Understanding the root cause of a blood disorder is the first step toward effective management. The "Great Divide" in hematology exists between conditions we are born with and those we develop over time.
Direct Answer: What causes chronic blood disorders?
Most chronic blood disorders are either inherited, resulting from genetic mutations passed down through families (such as Sickle Cell Disease, Thalassemia, and Hemophilia), or acquired later in life through autoimmune responses, certain medications, nutritional deficiencies, or underlying health conditions like kidney disease.
Inherited conditions often involve a permanent "instructional error" in the DNA responsible for producing red cells, white cells, or clotting factors. For families navigating these diagnoses, genetic counseling is a cornerstone of preventive care, providing a roadmap for future generations. On the other hand, acquired disorders can sometimes be triggered by external stressors. Drug-induced hemolytic anemia, for instance, occurs when the immune system mistakenly attacks its own red blood cells in response to a specific medication.
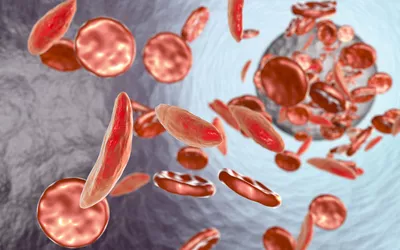
Identifying the Signs: Clotting vs. Bleeding Disorders
The human body acts as a "Living Sentinel," constantly monitoring its own integrity. When the blood's ability to flow or clot is compromised, the body sends specific, often contrasting, distress signals. Distinguishing between these two categories is vital for seeking the correct medical intervention.
Direct Answer: How can you distinguish between clotting and bleeding disorder symptoms?
Clotting disorders (thrombosis) often manifest as swelling, warmth, and tenderness in the limbs, alongside chest pain or shortness of breath. Conversely, bleeding disorders are characterized by frequent, unexplained bruising, prolonged bleeding from minor cuts, and chronic joint pain caused by internal hemorrhaging.
Symptom Contrast: Recognizing the Warning Signs
To help you monitor your health more effectively, consider the following comparison of how these conditions typically present:
| Symptom Category | Clotting Disorders (Thrombosis) | Bleeding Disorders |
|---|---|---|
| Physical Appearance | Redness, localized swelling (often in one leg), or skin that is warm to the touch. | Large or frequent bruises, small red spots on the skin (petechiae), and pale skin. |
| Internal Sensations | Sharp chest pain, sudden shortness of breath, or deep, aching pain in a limb. | Joint stiffness and throbbing pain (indicating internal bleeding), and chronic fatigue. |
| External Indicators | Vision changes or sudden weakness (if a clot affects blood flow to the brain). | Frequent nosebleeds, heavy menstrual cycles, and prolonged bleeding after dental work. |
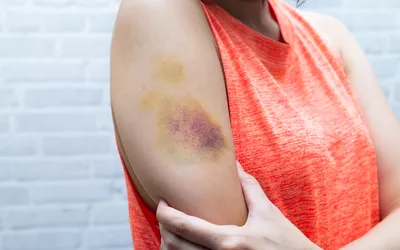
If you notice sudden swelling in a single limb accompanied by tenderness, it may indicate Deep Vein Thrombosis (DVT), a condition where a clot forms in a deep vein. This requires immediate attention to prevent the clot from traveling to the lungs.

Major Chronic Blood Conditions to Know
Moving "From Molecules to Medicine," it is essential to look at the most prevalent conditions that require long-term management strategies.
Anemia & Thalassemia: Red Cell Longevity
Anemia is perhaps the most ubiquitous blood disorder, affecting millions. It occurs when the body lacks enough healthy red blood cells to carry adequate oxygen to tissues. While dietary iron deficiency is a common cause, chronic forms like Thalassemia involve a genetic defect in hemoglobin production. Managing these conditions focuses on "oxygen transport optimization" through supplements, diet, and, in severe cases, regular transfusions.

Hemophilia (A & B): The Burden of Deficiency
Hemophilia is a rare but well-known inherited disorder where the blood doesn't clot properly due to a lack of specific clotting factors (Factor VIII or IX). Historically, this meant a life of restricted activity, but modern prophylactic treatments are "Rebalancing the Scale," allowing patients to lead active, fulfilling lives.
Platelet & Plasma Disorders
Conditions like Von Willebrand Disease (VWD) affect the proteins that help platelets stick together. Because VWD is often underdiagnosed, many people live for years with "silent" symptoms like heavy menstruation or easy bruising without realizing there is a manageable underlying cause.
Standard Treatment Options and Care Management
Managing chronic blood disorders is no longer a one-size-fits-all approach. It requires a multidisciplinary care team—including hematologists, specialized nurses, and physical therapists—to address both the physiological and lifestyle impacts of the disease.
Direct Answer: What are the most common treatments for chronic blood disorders?
Treatment is tailored to the specific disorder but typically includes factor replacement therapy for hemophilia, blood transfusions and folic acid for anemia, and anticoagulants (blood thinners) like Heparin or Lovenox for clotting disorders.
Modern care has also moved toward "Comprehensive Care Programs" that utilize telemedicine, allowing patients to consult with specialists from the comfort of home. This is particularly transformative for those with rare diseases who may live far from a specialized treatment center.
Advanced Strategies: The Evolving Treatment Landscape
For those living with hemophilia and related conditions, advanced hemophilia management strategies are rapidly evolving. The focus is shifting from "reactive" treatment (treating a bleed after it starts) to "proactive" stabilization.
- Factor VIII Mimetics & Bispecific Antibodies: New medications like Mim8 and NXT007 are designed to mimic the function of missing clotting factors. These can often be administered subcutaneously (under the skin) rather than through a vein, significantly reducing the treatment burden.
- Rebalancing Agents: These therapies, such as Concizumab and Marstacimab, work by targeting the body’s natural anticoagulants, essentially "fine-tuning" the blood's ability to clot without needing direct factor replacement.
- Extended Half-Life Products: These engineered proteins stay in the bloodstream longer, meaning fewer injections are needed to maintain safe factor levels, supporting more active and spontaneous lifestyles.
The Future: Bioelectric Medicine and 'Living Pharmacies'
As we look toward the next decade, the most exciting frontier is the concept of the "Living Pharmacy." Researchers are exploring the use of engineered cells that can be housed in miniature, implantable bioelectric devices. These devices would act as internal manufacturing plants, automatically releasing necessary proteins or factors into the bloodstream as needed.
This shift moves us away from monthly prescriptions and toward a "set and forget" model of healthcare. By reducing the frequency of medical interventions, we not only improve the quality of life for patients but also significantly lower long-term healthcare costs.
In the realm of preventive care, this means transitioning from managing a "disease" to maintaining "wellness." Through a combination of cutting-edge science, genetic understanding, and proactive lifestyle habits, the burden of chronic blood disorders is lighter today than ever before.
FAQ: Common Questions About Blood Disorders
Can lifestyle changes improve chronic blood disorders? While lifestyle changes like a nutrient-dense diet and regular exercise cannot "cure" genetic blood disorders, they are essential for preventive care. For instance, maintaining hydration and avoiding smoking can significantly reduce the risk of complications in clotting disorders.
How often should someone with a chronic blood disorder see a specialist? Most experts recommend a comprehensive review at a Hemophilia Treatment Center (HTC) or specialized hematology clinic at least once a year, even if symptoms are well-managed. These visits are crucial for adjusting dosages and screening for long-term complications like joint damage.
Are new treatments like gene therapy available for everyone? Gene therapy is an emerging field and is currently FDA-approved for specific types of Hemophilia B. However, eligibility depends on various factors, including the patient’s age, liver health, and the presence of certain antibodies.
Take Charge of Your Hematologic Health
Staying informed is the first step in self-care. If you or a loved one are managing a chronic blood condition, connecting with a specialized care team can provide access to the latest therapies and support systems.


