For many of us, the word "cancer" has historically been synonymous with a grueling battle of attrition—a journey defined as much by the toxicity of the treatment as by the disease itself. However, as we move through 2026, the narrative has fundamentally shifted. We are no longer in the era of "carpet-bombing" the body with systemic chemotherapy; we have entered the age of molecular precision. Today, the focus is not just on survival, but on the quality of that survival, treating the "risk" through interception and the disease through highly targeted biological interventions.
Executive Summary: The 2026 Modality Shift
What are the main cancer treatment modalities in 2026? Modern oncology has pivoted toward precision medicine. The primary pillars now include Immunotherapy (CAR-T, mRNA vaccines), Antibody-Drug Conjugates (ADCs), and advanced Radiation techniques like Proton therapy. These modalities are designed to target malignant cells with surgical accuracy while sparing healthy tissue, often moving care from the hospital ward to the outpatient clinic.
1. The New Pillars of Cancer Modality
The "Big Three" of traditional oncology—surgery, radiation, and chemotherapy—have been reimagined. In 2026, we think of treatment in terms of "biological missiles" and "living drugs."
Antibody-Drug Conjugates (ADCs): The Biological Missiles
ADCs represent one of the most significant breakthroughs in oncology. By linking a potent chemotherapy agent to a monoclonal antibody, these drugs act as a GPS-guided system. The antibody finds the specific protein on a cancer cell, docks, and releases the "payload" directly inside the tumor. This prevents the systemic "poisoning" effect of traditional chemo. New ADCs like ARB1002 are currently revolutionizing treatment for hard-to-reach cancers like pancreatic and HER2-low breast cancer, offering hope where options were once slim.
Immunotherapy 2.0: Beyond PD-1
While early immunotherapy focused on unlocking the immune system (checkpoint inhibitors), 2026 brings us Bispecific Antibodies and mRNA Therapeutic Vaccines. Unlike the COVID-19 vaccines that prevent infection, these therapeutic vaccines are personalized to a patient’s specific tumor mutations, "teaching" the immune system to recognize and destroy microscopic residual disease to prevent recurrence. This is particularly effective in melanoma and colorectal cancers.
Cellular Therapies: 'Living Drugs'
CAR T-cell therapy has matured into a standard of care for blood cancers. Long-term clinical data in 2026 shows that CAR T-cell therapy has achieved remarkable outcomes, with some patients maintaining remission for over 10 years. We are also seeing the rise of TIL (Tumor-Infiltrating Lymphocyte) therapy for solid tumors, where a patient’s own immune cells are harvested from their tumor, "supercharged" in a lab, and re-infused to finish the job.
2. Managing Side Effects through Precision
One of the most frequent questions I receive as an editor is: How do new cancer therapies reduce side effects compared to traditional chemotherapy?
The answer lies in molecular profiling. Traditional chemotherapy attacks all rapidly dividing cells, including those in your hair follicles, gut lining, and bone marrow. In contrast, 2026 therapies target specific genetic mutations unique to the cancer. This precision significantly reduces systemic symptoms like hair loss and severe nausea.
Furthermore, we now use the "Digital Twin" approach. Before a single drop of a high-toxicity drug is administered, AI models create a digital replica of the patient’s metabolism to predict how they will react. This allows oncologists to adjust dosages to the "Goldilocks" zone—effective enough to kill the cancer, but gentle enough to preserve the patient’s daily routine.
| Feature | Traditional Systemic Chemo | 2026 Targeted Infusions |
|---|---|---|
| Targeting | All fast-growing cells | Specific molecular/genetic markers |
| Delivery | Systemic (Entire body) | Localized or Antibody-guided |
| Common Side Effects | Nausea, Hair loss, Neuropathy | Fatigue, mild skin rash, localized inflammation |
| Treatment Setting | Often inpatient/Long infusions | Primarily outpatient/Short infusions |
| Recovery Time | Weeks/Months | Days |
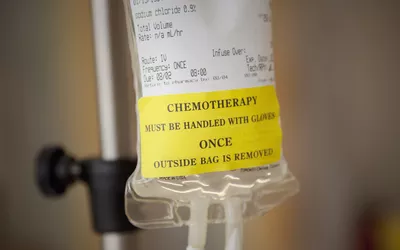
For those undergoing treatment, the focus has shifted toward proactive wellness. We no longer wait for side effects to appear; we intercept them. For instance, localized delivery systems like hepatic artery infusions allow for high-dose treatment in the liver while keeping the rest of the body safe.
Expert Forecast: "By the end of 2026, we expect a 40% increase in outpatient-based treatments for advanced cancers. This isn't just a logistical win; it’s a psychological one. Healing happens best when a patient can sleep in their own bed and maintain their family rituals." — Dr. Elena Vance, Oncology Research Lead.
3. Diagnostic Breakthroughs: Detection and Monitoring
We cannot treat what we cannot see. The diagnostic landscape of 2026 is defined by two words: Liquid Biopsies. Instead of invasive tissue biopsies, tests like the MSK-ACCESS use a simple blood draw to detect circulating tumor DNA (ctDNA).
These tests allow us to:
- Monitor in Real-Time: We can see if a treatment is working within weeks, rather than waiting months for a PET scan.
- Detect Minimal Residual Disease (MRD): We can find "invisible" cancer cells after surgery, helping us decide who actually needs adjuvant therapy and who can safely avoid it.
- AI Integration: AI algorithms now have a 70-80% accuracy rate in predicting which patients will respond to specific immunotherapies, saving precious time and resources.
4. Advanced Radiation and Surgical Techniques
The "blade and the beam" have also evolved. Proton Beam Therapy has become more accessible, offering sub-millimeter precision for tumors near critical structures like the brain, eye, or spine. Unlike traditional X-rays, protons stop at a specific depth, meaning there is zero "exit dose" to healthy organs behind the tumor.
In the operating room, Robotic-Assisted Surgery (using the Da Vinci 5 systems) has made "major" surgery "minor." With enhanced 3D visualization and tremor-filtering technology, surgeons can perform complex resections with minimal blood loss. For younger patients, this has been a game-changer for fertility preservation and faster returns to work.
5. The Survivorship Landscape and Global Access
Perhaps the most inspiring question to answer is: What is the outlook for metastatic cancer with modern immunotherapy?
Breakthroughs in immunotherapy have successfully extended survival for metastatic cancers, such as melanoma and certain lung cancers, from a few months to several years. In 2026, we are seeing patients achieve durable remission for over a decade. Metastatic cancer is increasingly being managed as a chronic condition—much like diabetes or hypertension—rather than a terminal diagnosis.
Expert Sidebar: Global Cost Comparison (2026) While these technologies are cutting-edge, global medical hubs have made them more accessible.
- CAR-T Therapy: $350k - $500k (USA) vs. $60k - $90k (India/Turkey)
- Proton Therapy: $30k - $50k per course (UK/EU) vs. $15k - $25k (Medical Hubs in SE Asia)
- Note: Always ensure international facilities are JCI-accredited and offer integrated follow-up care.

The 2026 oncology shift has resulted in a 40% increase in outpatient-based treatments for advanced cancers. This transition from systemic chemotherapy to targeted infusions like TILs and Proton therapy is not just about medical efficacy; it’s about restoring the patient's agency.
FAQ
Q: Are these 2026 treatments covered by standard insurance?
A: Most targeted therapies and ADCs that have FDA/EMA approval are covered, though personalized mRNA vaccines and certain CAR-T applications may still require clinical trial enrollment or specialized "high-tier" plans.
Q: Does "reduced side effects" mean "no side effects"?
A: No. While we’ve eliminated many traditional symptoms like severe hair loss, new therapies can cause "off-target" effects, such as inflammation or skin rashes. However, these are generally more manageable and less debilitating than the exhaustion of traditional chemo.
Q: How do I know if I’m a candidate for precision oncology?
A: Request a Comprehensive Genomic Profiling (CGP) test. This is the foundation of 2026 care, identifying the specific "drivers" of your cancer to see if a matching targeted therapy exists.
Conclusion: A New Horizon of Hope
Navigating a cancer diagnosis in 2026 is vastly different than it was even five years ago. We have moved from a "one-size-fits-all" approach to a bespoke model of care that honors the individual’s biology and lifestyle. While the journey remains challenging, the tools at our disposal are more powerful, more precise, and more humane than ever before.
If you or a loved one are facing a diagnosis, remember: Hope is no longer just a sentiment; it is backed by data. Seek out second opinions from centers that prioritize molecular profiling, and don't be afraid to ask about the latest ADC or immunotherapy options. Your path to wellness is being rewritten, one cell at a time.


