For many of us, our skin is more than just a protective barrier; it is a mirror reflecting our internal well-being. When that mirror shows the persistent, often painful patches of psoriasis, it can feel like our own body is speaking a language we don’t yet understand. Psoriasis is a chronic inflammatory skin condition driven by an overactive immune system that causes skin cells to multiply too quickly, resulting in scales and itchy, dry patches. Unlike a simple rash, it is a complex, systemic dialogue between our genetics, our environment, and our immune health.
Managing psoriasis requires us to look beyond the surface. While the visible plaques are the most immediate concern, true wellness comes from a holistic approach that balances modern clinical breakthroughs with mindful lifestyle adjustments. By understanding the "why" behind our flares, we can move from a state of reactive frustration to one of proactive care.
Understanding Psoriasis: More Than Just a Skin Condition
To truly manage psoriasis, we must first understand its biological rhythm. In a typical body, skin cells go through a life cycle of about 28 to 30 days—they grow deep within the skin, rise to the surface, and eventually shed. In a person with psoriasis, this process is accelerated to a staggering degree, often taking only three to four days. This rapid turnover is what leads to the buildup of "plaques"—thick, scaly patches of skin that the body simply cannot shed fast enough.
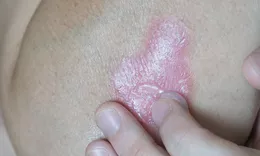
One of the most important things we need to communicate to the world—and remind ourselves—is that psoriasis is entirely non-contagious. You cannot "catch" it from someone else, nor can you spread it to others through touch. It is an immune-mediated disease, meaning the inflammation is coming from within. When our immune system becomes overactive, it sends out signals that trigger this rapid cell production. While it manifests on the skin, it is fundamentally a systemic condition.
Recognizing Symptoms Across Different Skin Tones
Psoriasis does not look the same on everyone. For years, medical textbooks focused primarily on how the condition appeared on lighter skin tones, but we now know that inclusivity in diagnosis is vital for effective treatment.
On lighter skin tones, psoriasis typically presents as well-defined red patches covered in silvery-white scales. However, on skin of color—including Black, Hispanic, and Asian individuals—the patches may appear purple, grayish, or even dark brown. These plaques may also be thicker and more likely to leave behind areas of temporary skin discoloration (post-inflammatory hyperpigmentation) once they heal.
Common sites for these plaques include the elbows, knees, and lower back, but "high-impact" sites can be particularly challenging. Scalp psoriasis, for instance, affects nearly 50% of patients and requires a different approach than body plaques due to the presence of hair and the sensitivity of the skin.
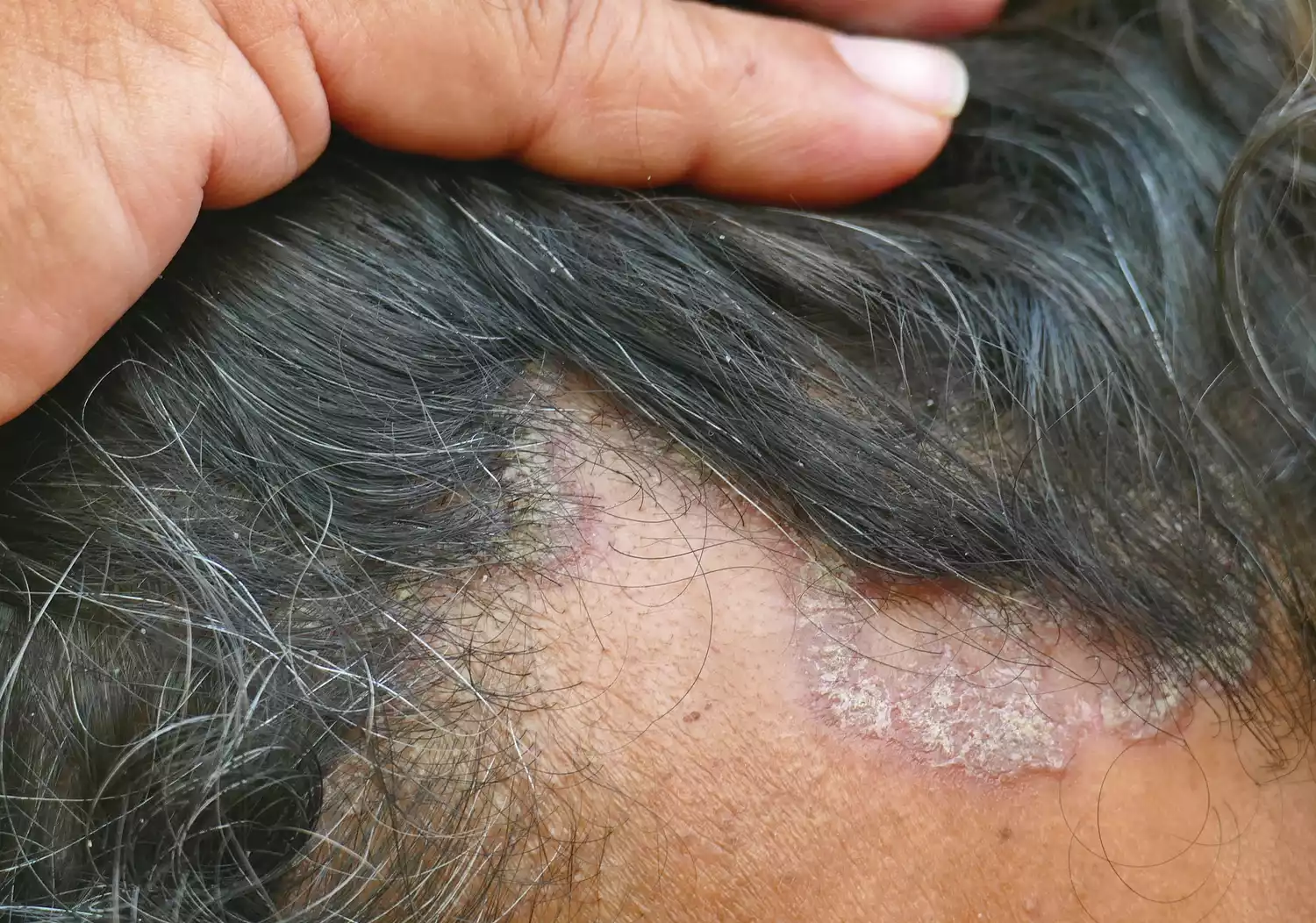
Beyond the visual markers, the physical sensation is often what impacts daily life the most. Patients frequently report a persistent itching, burning, or stinging sensation that can disrupt sleep and focus. In some cases, such as guttate psoriasis, the lesions appear as small, drop-shaped spots rather than large plaques, often triggered by a bacterial infection like strep throat.
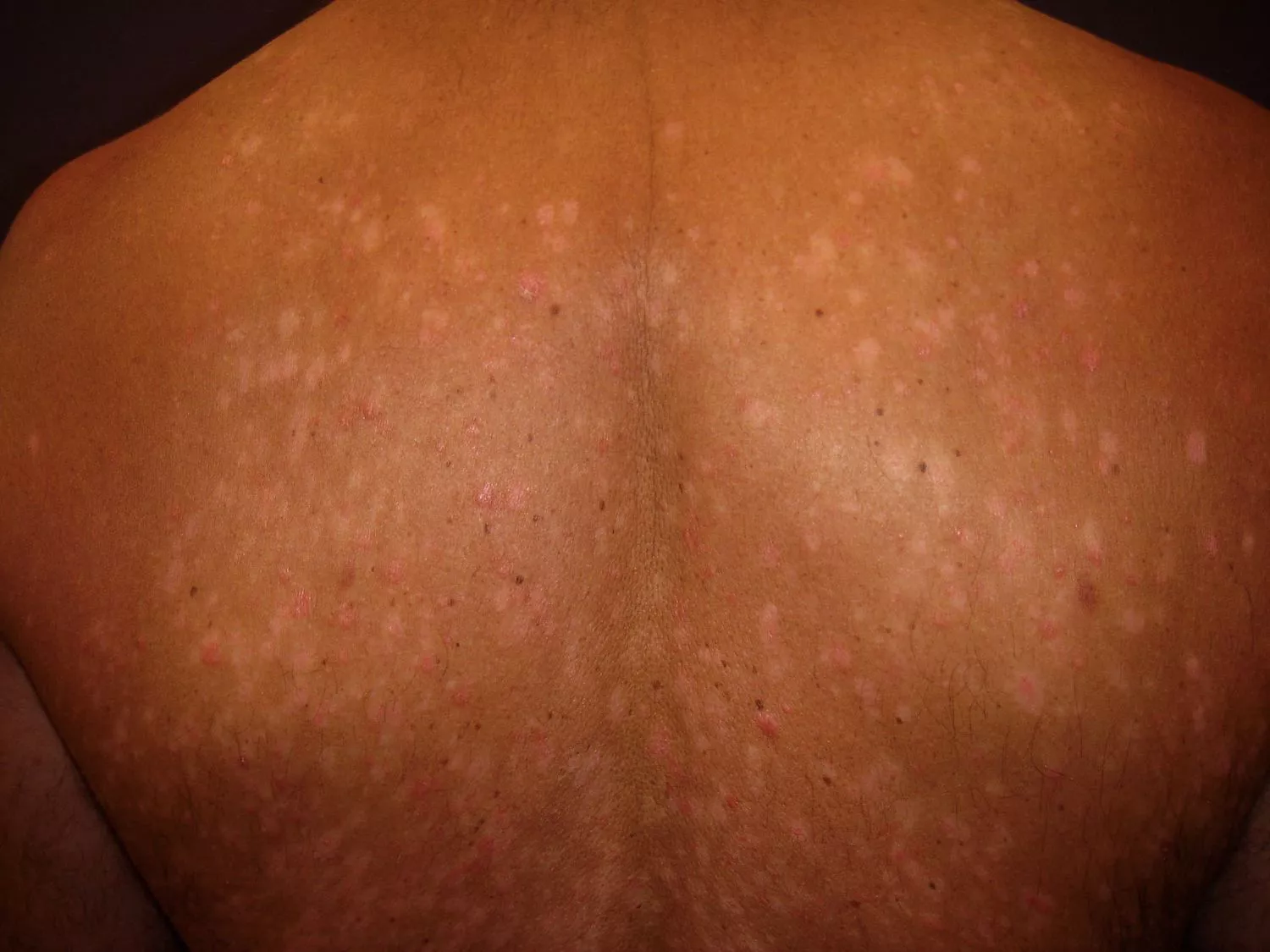
The Root Causes and Common Flare Triggers
While the exact "off switch" for psoriasis remains a subject of intense research, we know that genetics play a significant role. It isn't just about a single "psoriasis gene"; rather, it involves a complex interplay of inflammatory cells, particularly those originating in the bone marrow, that mistakenly target healthy skin cells.
However, genetics are only half of the story. Our environment and lifestyle choices act as the "on switch" for these genetic predispositions. Common lifestyle triggers for psoriasis flare-ups include high stress levels, smoking, alcohol consumption, cold/dry weather, and certain medications like beta-blockers or lithium.

We must also be mindful of the Koebner phenomenon. This occurs when a new psoriasis flare develops at the site of a skin injury—even a minor one like a scratch, a bug bite, or a new tattoo. This is why gentle skincare and the avoidance of harsh physical exfoliants are so critical for those in the community.
Editor’s Tip: During the winter months, the lack of humidity can strip moisture from the skin, making the Koebner phenomenon more likely. Investing in a high-quality humidifier for your bedroom can be a simple but effective preventive step.
Modern Clinical Treatment Options
The landscape of psoriasis treatment has shifted dramatically over the last decade. We have moved from simply "managing" symptoms to targeting the specific molecular pathways that cause the disease.
The Treatment Hierarchy
| Treatment Type | How it Works | Best For |
|---|---|---|
| Traditional Topicals | Steroids or Vitamin D3 analogues applied directly to the skin to reduce inflammation. | Mild to moderate localized plaques. |
| Phototherapy | Controlled exposure to Narrowband UVB light under medical supervision. | Moderate cases or when topicals fail; helps slow cell growth. |
| Biologics | Injectable proteins that target specific parts of the immune system (IL-17, IL-23). | Moderate to severe psoriasis; focuses on long-term remission. |
| Oral Systemics | Pills that work systemically to dampen the immune response. | Patients who prefer oral medication over injections. |
Modern clinical research has also brought us to the edge of a new era: nanomedicine. Emerging models of nanostructured topical gels featuring metal oxide nanoparticles show faster anti-inflammatory effects than traditional topical treatments. These "nanogels" are designed to penetrate the thick skin barrier of a plaque more effectively, delivering medication exactly where it is needed without the systemic side effects of high-dose steroids.
For those looking for the latest innovations, Phase III trials are currently underway for once-daily pills like icotrokinra, which targets the IL-23 receptor. These "oral biologics" represent a potential future where we can achieve the high clearance rates of injections with the convenience of a daily vitamin.
Holistic Management: Diet and Lifestyle Integration
As an advocate for preventive care, I believe that what we put into our bodies is just as important as what we put on them. While there is no "psoriasis diet" that works for everyone, the evidence for an anti-inflammatory approach is overwhelming.
Effective dietary strategies for psoriasis include adopting a Mediterranean diet rich in seafood, olive oil, leafy greens, and nuts. This way of eating naturally avoids inflammatory triggers like red meat, refined sugars, and highly processed oils. Clinical research indicates that anti-inflammatory supplements, particularly turmeric (curcumin) and omega-3 fatty acids (fish oil), provide the most convincing data for complementary psoriasis support. Omega-3s, in particular, help to lubricate the skin from the inside out and may reduce the redness and scaling associated with flares.

The Cortisol Connection
We cannot talk about psoriasis without talking about stress. Stress triggers the release of cortisol, which in turn can send the immune system into overdrive. Managing our "inner weather" through digital detoxing, meditation, and consistent sleep routines isn't just about mental health—it's a clinical necessity for skin clearance. When we lower our systemic stress, we lower our systemic inflammation.
The Importance of Managing Comorbidities
Psoriasis is not just a skin disease; it is a systemic inflammatory condition. Because the inflammation that affects the skin can also affect other parts of the body, we must be vigilant about our overall health.
- Cardiovascular Health: Persistent internal inflammation is a known risk factor for heart disease. It is essential for psoriasis patients to have yearly lipid panels and blood pressure checks. Studies have shown that effectively treating psoriasis can actually lower the risk of heart attack and stroke.
- Psoriatic Arthritis: Roughly 1 in 3 people with psoriasis will develop psoriatic arthritis (PsA). If you notice morning stiffness or "sausage-like" swelling in your fingers or toes, consult a rheumatologist immediately. Early intervention is key to preventing permanent joint damage.
- Mental Well-being: There is a profound link between skin conditions and mental health. The visibility of psoriasis can lead to social anxiety, while the systemic inflammation itself is linked to higher rates of depression. Seeking support from a therapist or a support group is not a sign of weakness; it is a vital part of a holistic treatment plan.
Did You Know? Patients who achieve "clear" or "almost clear" skin through modern treatments often report a significant improvement in their overall quality of life scores, showing how closely our skin health is tied to our emotional resilience.
FAQ
Q: Can psoriasis be cured completely? A: Currently, there is no permanent "cure," but we have reached a point in medicine where "clear skin" is a realistic and achievable goal for the majority of patients through a combination of biologics, topicals, and lifestyle changes.
Q: Is it safe to use natural oils like coconut or tea tree oil? A: Natural oils can be excellent for moisturizing and softening scales (keratolytic effect). However, they do not treat the underlying immune cause. Always patch-test new products to ensure they don't trigger a flare.
Q: How does weather affect my skin? A: Most people find that cold, dry weather triggers flares, while moderate sun exposure (UVB rays) can actually improve symptoms. However, always consult your dermatologist before starting "natural" sun therapy to avoid the risk of burning.
Your Path Forward
Living with psoriasis is a journey of constant adjustment, but you are not traveling it alone. By combining the precision of modern medicine with the wisdom of a holistic lifestyle, you can reclaim control over your skin and your health.
If you are feeling overwhelmed by a recent flare or are looking to update your treatment plan, I encourage you to reach out to a board-certified dermatologist who specializes in immune-mediated conditions. Together, you can build a routine that honors both your body’s needs and your lifestyle goals.


