When the conversation shifts from curative treatments to comfort care, the air in the room often feels heavy with a mixture of grief, exhaustion, and a profound, quiet love. As a mental health editor, I have sat with many families navigating this threshold. The transition from fighting a disease to honoring a life is perhaps the most difficult journey a caregiver will ever take. Understanding late-stage lymphoma symptoms and the clinical markers of progression isn't just about medical preparedness; it is about reclaiming a sense of agency in a situation that feels out of control. It allows you to move from a state of reactive fear to one of mindful presence, ensuring your loved one’s final days are defined by dignity and peace rather than crisis.
Navigating the Transition to Comfort Care
The decision to move toward palliative or hospice care is rarely a single event. It is often a gradual realization that the body is tired, and the burdens of aggressive treatment have begun to outweigh the benefits. In the final stages of lymphoma, the goals of medicine shift. We stop asking "How can we stop the cancer?" and begin asking "How can we maximize comfort, connection, and emotional well-being?"
This shift is an invitation to practice radical presence. For the patient, it is a time of letting go; for the caregiver, it is a time of "holding space." Acknowledging the emotional landscape—the anger at the disease, the fear of the unknown, and the anticipatory grief—is the first step in providing high-quality care. By understanding what to expect, you can reduce the "shock of the new" and focus on the quiet moments that matter most.

Identifying Physical Signs of Final-Stage Lymphoma
As lymphoma progresses, the body begins a natural process of shutting down. While every person’s journey is unique, clinical observations have identified six primary physical markers that signify terminal progression. Recognizing these signs of dying from lymphoma helps caregivers provide the right environment for comfort.
- Profound Fatigue and Lethargy: This is perhaps the most universal sign. The patient may spend the vast majority of the day sleeping and may eventually become difficult to rouse. This is not "laziness" or a lack of will; the body is simply conserving its remaining energy for vital internal processes.
- Loss of Appetite and Weight Loss: The metabolic needs of the body decrease significantly. Patients often lose interest in food and water. Forcing a loved one to eat at this stage can actually cause physical distress, such as nausea or bloating.
- Respiratory Changes: Breathing becomes more shallow, labored, or irregular.
- Neurological Shifts: Confusion, disorientation, or a withdrawal from social interaction are common.
- Temperature Sensitivity: The body’s internal thermostat begins to fail. You may notice the person’s hands and feet feel cold to the touch, or they may experience bouts of sweating.
- Loss of Bodily Control: This includes both a loss of bowel/bladder control and a general inability to move or reposition themselves without help.

Clinical Markers and Skin Changes
In addition to the primary markers, dermatological changes are frequently observed. Because the heart is no longer pumping blood as effectively to the extremities, the skin may appear mottled (purplish or blue patterns), particularly on the undersides of the arms, legs, and feet. You may also see lymphoma-specific rashes or skin lesions that become more prominent as the immune system wanes.
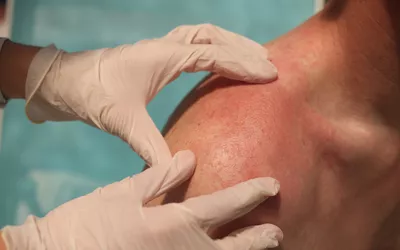
Pro Tip: To manage temperature sensitivity, avoid using heavy electric blankets, which can be difficult for the patient to adjust. Instead, use layered light blankets and focus on gentle skin care to prevent dryness or irritation.
Understanding Neurological & Sensory Shifts
The neurological impact of advanced lymphoma can be particularly distressing for family members. Lymphoma, especially cases involving the Central Nervous System (CNS), can lead to significant cognitive changes.
Patients often experience "terminal restlessness," which manifests as picking at bedsheets, trying to get out of bed despite weakness, or general agitation. This is frequently a result of metabolic changes or the brain’s reaction to declining oxygen levels.
- Confusion and Disorientation: The patient may not know where they are or may confuse the past with the present.
- Social Withdrawal: As energy levels drop, patients often stop speaking or acknowledging those in the room. This is a natural "turning inward" and should not be taken as a rejection of your presence.
- Visions and Hallucinations: It is common for patients to speak to or see people who have already passed away. From a psychological perspective, these "visions" often provide comfort to the dying, and it is usually best to listen and validate their experience rather than trying to correct them with "facts."
Managing Respiratory Changes and the 'Death Rattle'
One of the most concerning lymphoma end of life expectations for caregivers is the change in breathing patterns. As the body nears the end, the muscles used for breathing relax, and the reflex to clear the throat weakens.
The Mechanism of Breathing Changes
- Apnea: You may notice periods where the patient stops breathing for several seconds, followed by a series of rapid breaths. This is known as Cheyne-Stokes breathing and is a normal part of the dying process.
- The 'Death Rattle': This is a rattling or gurgling sound caused by the accumulation of secretions in the back of the throat. While the sound can be distressing to listeners, clinical evidence suggests the patient is generally not in distress or "drowning."
- Air Hunger: Some patients may look as though they are gasping for air. This "dyspnea" can often be managed with low-dose morphine or oxygen therapy provided by hospice nurses.
Comfort Measures for Breathing:
- Positioning: Elevate the head of the bed or use pillows to prop the patient up at a 45-degree angle.
- Cool Air: A small fan blowing gently across the face can reduce the sensation of "air hunger."
- Moisture: Use a damp cloth or mouth swabs to keep the lips and mouth moist, as mouth-breathing causes significant dryness.
Palliative vs. Hospice Care: Choosing the Best Support
Many people use these terms interchangeably, but they represent different stages of the support journey. Understanding the distinction is vital for ensuring your loved one receives the appropriate level of care.
| Feature | Palliative Care | Hospice Care |
|---|---|---|
| Eligibility | Any stage of a serious illness. | Terminal diagnosis (life expectancy < 6 months). |
| Treatment Focus | Can be combined with curative treatments. | Focuses solely on comfort; curative treatments stop. |
| Location | Hospitals, clinics, or home. | Most often provided at home or in a dedicated facility. |
| Goal | To improve quality of life and manage symptoms. | To provide a "good death" and support the family. |
Hospice care is a philosophy, not just a place. Choosing home-based hospice allows for a familiar environment, surrounded by the sights and smells of home, which can significantly reduce the patient's anxiety and disorientation.
Practical Planning: Advanced Directives and Financial Matters
In my work, I find that much of the "background anxiety" caregivers feel stems from the fear of not knowing the patient’s final wishes. Addressing these logistics early—though difficult—is an act of profound love and mindfulness. It clears the path for emotional connection later.
Essential Documentation
Ensure you have a Living Will and a Medical Power of Attorney (POA). These documents stipulate exactly what kind of interventions the patient wants (e.g., Do Not Resuscitate orders) and who is authorized to make decisions when the patient can no longer speak for themselves.

Financial and Final Arrangement Estimates
While it feels cold to discuss costs, the reality of the 2025 economic landscape means that being prepared can prevent future financial trauma.
- Average Burial Costs (2025): Starting at approximately $2,636 (basic services, not including casket or plot).
- Average Cremation Costs (2025): Starting at approximately $2,202.
Keep all important documents—insurance policies, bank info, and legal forms—in a fireproof box or a secure digital vault accessible to the designated POA.
Supporting the Caregiver: Managing Grief and Loss
As you care for someone with advanced lymphoma, you are also experiencing "caregiver burnout" and "anticipatory grief." You cannot pour from an empty cup. It is essential to recognize that your feelings—whether they are deep sadness, numbness, or even a sense of relief that the struggle is ending—are all valid.
- Physical Manifestations: Grief isn't just "in your head." It shows up as digestive issues, headaches, and extreme exhaustion.
- Finding Community: You are not alone. Organizations like Lymphoma Canada or Blood Cancer UK offer support groups specifically for those in the end-of-life caregiving phase.
- Helping Children: Use clear, age-appropriate language. Avoid euphemisms like "going to sleep," which can create fear of bedtime. Use words like "dying" and "the body has stopped working" to provide clarity.
FAQ: Frequently Asked Questions
Q: How long does the final stage of lymphoma last? A: The timeline varies, but the "active dying" phase—marked by the inability to swallow and significant breathing changes—usually lasts from a few days to a week. The broader "end-of-life" phase can last several weeks as the body gradually slows down.
Q: Is the 'death rattle' painful for the patient? A: No. While the sound is difficult for family members to hear, the patient is typically in a state of deep unconsciousness and is not bothered by the secretions. Repositioning the patient on their side can often help quiet the sound.
Q: What should I do if my loved one starts having hallucinations? A: Stay calm and present. If the visions are not distressing to them, there is no need to intervene. Simply sit with them and ask them to tell you about what they see. If the hallucinations cause fear or agitation, consult your hospice nurse about medication to ease the anxiety.
Conclusion
Navigating the final stages of lymphoma is a journey of the heart as much as it is a medical process. By understanding the late-stage lymphoma symptoms and the physiological shifts taking place, you can move away from the "fear of the unknown" and into a space of compassionate presence.
Remember that your presence is the greatest gift you can offer. You don't need to have all the answers or say the "perfect" thing. Simply being there—holding a hand, playing favorite music, or sharing a quiet memory—is enough. You are doing the hard, holy work of walking someone home.


