Imagine your body’s immune system as a highly trained security force. Its sole purpose is to identify and neutralize external threats like bacteria, viruses, and toxins. But in the case of Multiple Sclerosis (MS), this security force suffers from a profound case of mistaken identity. Instead of targeting a virus, it turns its weapons against the very structure that allows your brain to communicate with your body: the myelin sheath.
This biological error is not a rare occurrence; multiple sclerosis affects approximately 2.8 million people worldwide. For the majority of these individuals, the journey begins with myelin-attacking relapses that can eventually progress to permanent neurodegeneration. Understanding why this "friendly fire" happens is the first step in navigating the complexities of the disease. In this guide, we will explore the mechanisms of the Central Nervous System (CNS) immune attack, the reasons behind the immune system’s confusion, and the future of repairing the damage.
Understanding the Target: What is Myelin?
To understand why the attack is so devastating, we must first understand what is being destroyed. In the central nervous system—comprising the brain and spinal cord—nerve fibers called axons act as the long-distance cables for electrical signals. For these signals to travel fast enough to allow you to walk, talk, or blink, they require insulation.
This insulation is the myelin sheath, a protective protein and fatty coating that wraps tightly around the axons. Think of it like the plastic coating on a copper electrical wire. Without it, the "electricity" or nerve impulses leak out. When demyelination occurs in MS, the electrical signals traveling along the nerves are slowed, distorted, or completely blocked.
While the peripheral nervous system (the nerves in your limbs) can often repair its own myelin, the central nervous system has a much harder time. Over time, the loss of this protective coating leaves the underlying axon vulnerable. Chronic damage to these fibers eventually leads to the death of the nerve cells themselves, a process that underpins the long-term disability seen in progressive forms of the disease.
The Mechanism of Attack: T-Cells, B-Cells, and the Blood-Brain Barrier
The immune attack in MS is a multi-stage process that involves a breach of one of the body’s most secure borders: the Blood-Brain Barrier (BBB). In a healthy body, the BBB acts as a filter, allowing nutrients into the brain while keeping harmful cells and pathogens out. In MS, this barrier becomes "leaky."
The assault is orchestrated primarily by two types of white blood cells:
- T-Cells: These cells are essentially the "generals" of the immune system. In MS, certain T-cells become sensitized to myelin proteins. Once they cross the BBB, they release pro-inflammatory chemicals (cytokines) that recruit other immune cells to the site, triggering an inflammatory cascade.
- B-Cells: Once thought to be minor players, B-cells are now known to be central to the MS mechanism. They produce antibodies that specifically target the myelin sheath and provide "instructions" to other immune cells to intensify the attack.
Once the attack begins, local immune cells in the brain, known as microglia, and recruited macrophages begin to physically strip the myelin away from the axons. This creates an area of intense inflammation known as a lesion.
The Aftermath: Sclerosis and Cortical Atrophy
The term "Multiple Sclerosis" literally translates to "many scars." When the inflammatory attack subsides, the body attempts to heal, but the result is often the formation of tough, scar-like tissue or plaques. These areas of sclerosis are what neurologists look for during diagnostic imaging.
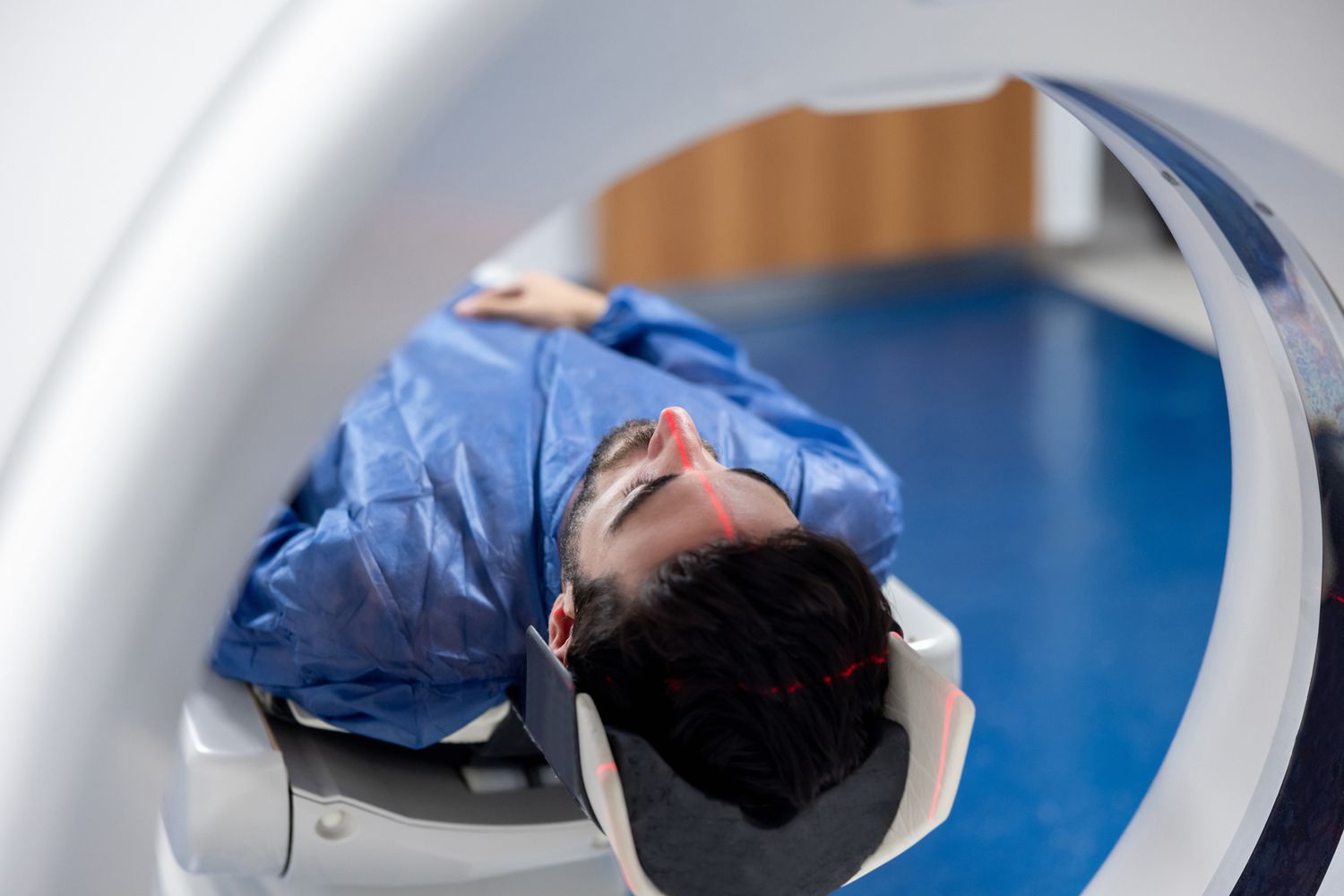
Identifying these lesions via MRI is a sophisticated process. Modern imaging looks for specific markers like the Central Vein Sign (a small vein visible in the center of a lesion) or Paramagnetic Rim Lesions, which indicate ongoing, chronic inflammation at the edges of a scar.
However, the damage isn't just limited to visible spots on a scan. Clinical research indicates that cortical atrophy, or the shrinking of the brain's outer layer, can occur at a rate up to 3 times faster in MS patients than in healthy individuals. This is due to the cumulative effect of chronic myelin loss and the eventual death of the underlying axons.
Comparing the Courses of Multiple Sclerosis
MS does not follow the same path for everyone. The way the immune system behaves dictates the "type" of MS a patient is diagnosed with:
| MS Type | Primary Characteristics | Progression Pattern |
|---|---|---|
| Relapsing-Remitting (RRMS) | The most common form (85%). Defined by clear attacks (relapses) followed by periods of partial or complete recovery. | Sudden onset of symptoms with long periods of stability between attacks. |
| Secondary Progressive (SPMS) | Often follows RRMS. The disease begins to progress more steadily with or without distinct relapses. | A transition from "attacks" to a slow, steady decline in function. |
| Primary Progressive (PPMS) | Affects about 15% of patients. Characterized by worsening neurological function from the beginning. | No distinct relapses or remissions; a steady accumulation of disability. |
Why Me? Triggers for the Immune Confusion
If the immune system is designed to protect us, why does it suddenly decide that myelin is an enemy? Scientists believe MS is caused by a complex "perfect storm" of factors rather than a single cause.
- Genetic Susceptibility: While MS is not directly hereditary, there are over 200 "susceptibility genes" related to immune function that can increase the risk of developing the disease.
- The Epstein-Barr Virus (EBV) Connection: Recent landmark studies have found that infection with EBV (the virus that causes mononucleosis) is likely a necessary trigger for MS. It is believed that the immune system, while trying to fight EBV, accidentally begins to recognize myelin proteins as looking similar to the virus—a phenomenon called "molecular mimicry."
- Environmental Factors: Sunlight and Vitamin D play a significant role. There is a documented "Latitudinal Gradient," where MS prevalence increases the further you move away from the equator. Low Vitamin D levels are associated with a higher risk of immune dysregulation.
- Lifestyle Impact: Smoking is a major risk factor. It not only increases the likelihood of developing MS but also exacerbates myelin damage and accelerates brain shrinkage.
Red Flag Symptoms: While many conditions cause fatigue or tingling, MS is often distinguished by "optic neuritis" (blurred vision or pain in one eye), "Lhermitte’s sign" (an electric-shock sensation that runs down the spine when bending the neck), and "Uthoff’s phenomenon" (worsening of symptoms when the body gets overheated).
Current Treatment: Managing the Immune Response
For decades, the goal of MS treatment has been immunomodulation—essentially "calming down" the immune system or preventing it from reaching the brain. These are known as Disease-Modifying Therapies (DMTs).
Current strategies include:
- Sequestration: Medications like Fingolimod trap immune cells in the lymph nodes so they cannot enter the bloodstream and cross the BBB.
- Depletion: Infusion therapies like Ocrelizumab target and remove specific B-cells that are responsible for the attack on myelin.
- BTK Inhibitors: A new class of drugs, such as Tolebrutinib, is currently being tested. Unlike older drugs, these can cross the BBB to target the "smoldering" inflammation inside the brain that causes progressive disability.
Selecting the right DMT is a collaborative process between the patient and their neurology team, often balancing the potency of the drug with its potential side effects.
The Next Frontier: Remyelination and Repair
While current treatments are excellent at preventing new damage, they do very little to fix the damage that has already occurred. This is the "Holy Grail" of MS research: remyelination.
The future of MS care is shifting from suppression to restoration. Scientists are investigating ways to stimulate oligodendrocytes (the cells responsible for making myelin) to go back to work and repair the "leaky" insulation on damaged axons.
Breakthrough research has identified specific compounds, such as K102 and K110, that appear to promote this repair process in preclinical models. If successful in human trials, these treatments could restore functional vision and nerve health, potentially reversing some of the disabilities caused by years of demyelination.
FAQ
Can myelin grow back on its own? In the early stages of MS, the body does have a limited ability to repair myelin (remyelination). This is why people with Relapsing-Remitting MS often recover from their initial attacks. However, as the disease progresses, the repair cells (oligodendrocytes) become exhausted or are prevented from working by scar tissue, leading to permanent damage.
Does an MS diagnosis mean I will eventually need a wheelchair? Not necessarily. Due to the advent of highly effective Disease-Modifying Therapies (DMTs), the long-term outlook for MS patients has improved dramatically over the last 20 years. Many people diagnosed today will live full, mobile lives with minimal disability, especially if they begin treatment early.
Why does heat make MS symptoms worse? This is known as Uthoff’s phenomenon. When the body temperature rises (due to exercise, a hot bath, or fever), it becomes even harder for electrical signals to travel across a demyelinated nerve. It’s not a "new" attack, but rather a temporary "short circuit" that usually resolves once the body cools down.
Taking Control of Your Journey
Understanding the "why" behind the immune system's attack on myelin is empowering. While we cannot yet "cure" the underlying autoimmune error, we have more tools than ever to manage the response, protect the brain, and look toward a future of repair.
If you or a loved one are experiencing neurological symptoms, the most important step is early intervention. Consult with an MS specialist to discuss advanced imaging and the latest therapeutic options.


